Radical Prostatectomy
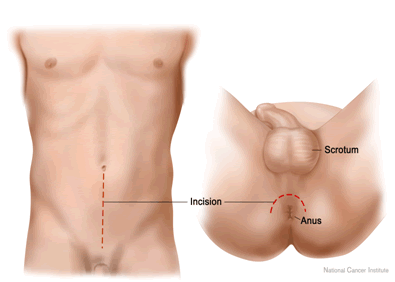
This operation involves the removal of the entire prostate gland together with the tissue immediately surrounding it. It is usually done retropubically, ie through an incision in the lower part of the abdomen. Sometimes it is carried out through the perineum (between the scrotum and anus) or laparoscopically. Laparoscopic radical prostatectomy is not widely performed and has not been shown to have better outcomes. Indeed there is a particular advantage of an open approach in that the prostate can directly be felt and any possible protrusions of the cancer through the capsule can be accommodated for. Whichever approach is used, there is usually a speedy postoperative recovery with the patient going home soon after surgery. A catheter is placed in the bladder at the time of surgery and patients go home with this in place and return usually after 2 weeks for it to be removed.
Most men do very well with surgery both in terms of recovering quickly but also in terms of cancer control. The serum PSA is measured 2 months post surgery and regularly thereafter (every few months).
About a third of men experience some incontinence in the immediate post-operative period. This improves over the ensuing weeks and months in almost everybody but there is a small proportion (about 5%) of men who complain of long term problems. This group may require other therapies in order to improve matters for them.
An additional complication of surgery (and radiotherapy) is impotence. As long as the disease is low stage a nerve-sparing radical prostatectomy is performed with the explicit aim of preserving erectile function.

